Oral Glandular Tissue (saliva secreting)
Begins development at 6 weeks gestation and is completed by about the 12th week
• Hydrating–moisturizing
• Cleansing
• Lubrication
• Digestion
• Remineralization of dentition(pH maintenance, buffering)
• Immunity mediator
• Antimicrobial (antifungal, antibacterial)
• Stimulation of minor salivary glands
• Cellular maintenance
• Enables swallowing
• Enables tasting
Enables speech articulation
Mechanisms of Salivary Production
Sympathetic-Causes very dry, thick, ropy saliva
Parasympathetic-Causes thin, watery, profuse salivation
The two divisions work in opposition and have the ability to physiologically alter the quality as well as the quantity of the saliva
Salivary Gland Classifications by Secretion
• Serous: very thin and watery
o parotid gland
o lingual glands of von Ebner (serous glands of von Ebner)
• Mucous: very thick and viscous
o palatine glands
o posterior lingual glands
o labial buccal glands
• Mixed secretions: mix of the two
• Sublingual glands
Mostly mucous with some serous
• Submandibular glands
Mostly serous with some mucous
• Anterior lingual glands
Mixed secretion
Salivary Gland Classifications by Major or Minor Glands
• Major glands
o Secrete saliva intermittently
• Minor glands
o Secrete saliva continuously
The Major Glands
• Parotid gland
o Largest of the 3 major glands
o Produces 30% of total saliva output
§ Parotid duct is also known as Stenson’s duct
- Parotid/Stenson’s duct exits opposing the maxillary second molar
o Located anterior but inferior to the external auditory meatus
o Innervated by sympathetic and parasympathetic divisions
o Secretes serous type saliva
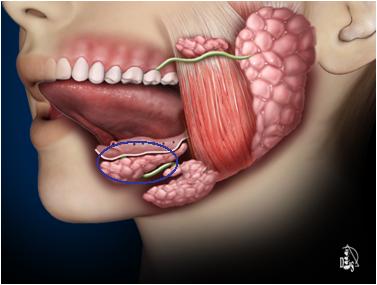
• Submandibular gland
o Second largest salivary gland
o Produces 65-70% of total saliva output
o The duct is called Wharton’s duct
o Wharton’s duct exits on the floor of the mouth opposing the lingual surface of the tongue
o Located in a depression on the lingual side of the mandibular body
o Innervated by parasympathetic nerve endings and possesses NO sympathetic receptors
o The parasympathetic fibers arrive through the facial and glossopharyngeal nerves
o Mixed secretion – mostly serous
• Sublingual glands
o Smallest of the major glands
o Produce less than 5% of total saliva output
§ Saliva delivered via the ducts of Bartholin
§ The Bartholin ducts exit on the base of the lingual surface of the tongue
o Innervated by parasympathetic fibers
o Little or no sympathetic influence
o Mixed secretion – mostly mucous
The Minor Salivary Glands
Minor salivary glands are found throughout the mouth:
– Lips
– Buccal mucosa (cheeks)
– Alveolar mucosa (palate)
– Tongue dorsum and ventrum
– Floor of the mouth
Together, they play a large role in salivary production.
Salivary Flow
• Unstimulated Flow (resting salivary flow―no external stimulus)
o Typically 0.2 mL – 0.3 mL per minute
o Less than 0.1 mL per minute means the person has hyposalivation
§ Hyposalivation – not producing enough saliva
• Stimulated Flow (response to a stimulus, usually taste, chewing, or medication [eg, at mealtime])
o Typically 1.5 mL – 2 mL per minute
o Less than 0.7 mL per minute is considered hyposalivation
• The average person produces approximately 0.5 L – 1.5 L per day
• Salivary flow peaks in the afternoon
• Salivary flow decreases at night when the parotid gland shuts down
• There is a difference in the quality between stimulated and unstimulated saliva
Salivary Composition
• 90% of saliva is water
• 10% is composed of inorganic and organic ions, and cellular components
o sodium, potassium, and calcium are positive ions (cations)
o chloride, bicarbonate, and phosphates are negative ions (anions)
• The cationic and anionic components play an important role in the function of saliva
Ions and Salivary Flow
As saliva passes through the salivary ducts, cations (sodium and chloride) are reabsorbed into the adjacent blood vessels.
As saliva passes through the salivary ducts, cations (sodium and chloride) are reabsorbed into the adjacent blood vessels. In exchange, bicarbonates and potassium are transferred from the blood vessels into the salivary ducts.
Stimulated Salivary Flow
• Saliva passes through the salivary duct very rapidly (a negative result of fast flow)
o It impedes the exchange of sodium and chloride for potassium and bicarbonate
Unstimulated Salivary Flow
• Has a high content of potassium and bicarbonate (a positive result of slow flow)
o The quality of unstimulated saliva will change when flow increases because of a stimulus (chewing gum, thinking about lemons, looking at a food you crave)
Fluoride and Saliva
Fluoride is also secreted in saliva.
Unlike the ions in saliva, the fluoride content (level) is not altered whether the salivary flow is simulated or unstimulated.
Organic Components of Saliva
Enzymes:
- Amylase – converting starch into glucose and fructose
- Lysozymes – prevents bacterial infections in the mouth
- Histatins – prevents fungal infections
- Secretory IgA – immunity mediator
- Lactoperoxidases – stimulation of minor salivary glands
- RNase and Dnase – cellular maintenance
- Lipase – initiates digestion of fat
- Kallikrein – vasoreactive substances
Cellular Composition of Saliva
The cellular composition consists of:
- Epithelial cells
- Neutrophils
- Lymphocytes
- Bacterial flora
Factors that Affect Salivary Flow
• Medication
• Autoimmune disease (Sjogren’s syndrome, lupus)
• Systemic diseases (diabetes, asthma, kidney, sarcoidosis, HIV)
• Stress/anxiety/depression
• Radiation therapy to the head and neck
– 30 Gy = glandular fibrosis (gland can still produce some saliva)
– 60-70 Gy = glandular destruction (gland can no longer produce saliva)
• Gender (70 % female, usually postmenopausal)
• Sympathomimetic medications (stimulate the sympathetic nervous system)
• Parasympatholytic medications (inhibit the parasympathetic nervous system)
• Circadian rhythms (decreases in the fall and increases in the spring)
Over 400 Medications Can Produce the Side Effect of Xerostomia
• Antacid
• Antianxiety
• Anticholinergic
• Anticonvulsant
• Antidepressant
• Antiemetic
• Antihistamine
• Antihypertensive
• Antiparkinsonian
• Antipsychotic
• Bronchodilator
• Cholesterol reducing
• Decongestant
• Diet pills
• Diuretic
• Hormonal replacement therapy
• Muscle relaxant
• Narcotic analgesic
SALIVARY GLANDS LECTURE NOTE....PPT
Salivary Gland Diseases.... Download ppt lecture note









thanks a lot...awsom stuff..!1
ReplyDeleteProto-col Slim-Fizz is a special appetite suppressant which is containing the ground-breaking fibre Glucomannan, which is a natural dissolvable fibre derived from pure Konjac.
ReplyDeleteI have been interested in facial creams for years, but could never find one that actually did what it said it would do. I was skeptical of Bio France Lab because it really did not have any reviews, but after ordering I am shocked! This is the best face cream I have ever used. It covers up all my blemishes and acne scars. I was worried, because it did not have any SPF, but I found out that it doesn't need any. I really don't want anyone to get this product because I want to keep it all to myself, but I strongly recommend it to anyone who is looking for a high quality face cream. I am getting one for my mother in law for mother's day. I feel like she will love it just as much as I do.
ReplyDelete