Clinical steps for
removable partial dentures
1. Assessment and
treatment plan.
2. Prelimary
impressions
These are usually taken using
alginate in a stock tray. For distal extension edentulous areas (Kennedy Class
I and II), modify the tray first with compound or silicone putty.
3. Occlusal record
If MIP (Maximal Intercuspal Position) is obvious, the
occlusion can be recorded conventionally at the same visit as first
impressions. If MIP is not obvious, occlusal rims (wax record blocks) will be
required, as will a separate visit. Where there are no teeth in occlusal
contact, the steps involved are the same as for recording the occlusion for F/F
(full upper and lower dentures) . If
there is an occlusal stop but insufficient standing teeth to produce a stable
relationship of the casts, the procedure is as follows:
- Determine the VDO (Vertical Dimension Of
Occlusion) and mark the position of two
index teeth with pencil.
- Define the arch form and occlusal plane using the
occlusal rim on which this is easiest, e.g., tooth to tooth, tooth to
retromolar pad.
- Check the occlusal rim in the mouth, using the mark on
the index teeth as a guide, and adjust blocks if necessary.
- Record occlusion with bite-recording paste or wax.
- Check that the relationship of the index teeth on the
articulated casts corresponds to that in the mouth.
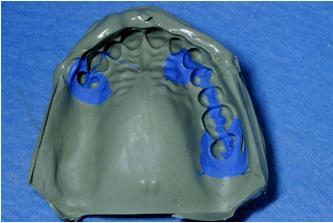
4. Survey mounted
casts and design denture

Surveying
A dental surveyor should be used to
determine heights of contour with a common path of insertion.
Objectives
- Establish path of insertion.
- Define those undercuts that may be used to retain
denture.
- Define those undercuts that require blocking out prior
to finish.
If the path of insertion is at 90°
to the occlusal plane insertion of the denture will be straightforward;
however, where the teeth are tilted or few undercuts exist, an angulated path
of insertion may be advantageous. Which path provides more resistance to
displacement during function is controversial.
A survey line can then be marked on
the teeth to indicate their height of contour in the plane of the path of withdrawal.
5. Tooth preparation
may be required to:
- Accommodate rest seats. Rests need to be >1 mm for
strength, ∴ if insufficient room in occlusion to accommodate this
bulk, tooth reduction is required.
- Establish guide planes
- Modify unfavorable survey line, e.g., ↓ height of
contour
6. Final impressions
using a custom tray.
Alginate is the most commonly used
material, but elastomers are preferable for deep undercuts. It is helpful to
have a wax try-in before the framework is made. This enables you to confirm
tooth position so that the retentive elements for the acrylic are placed
appropriately.
7. Framework try-in
- Check extension, adaptation, and position of clasp, and
rests. If casting does not fit, use of correcting fluid or a fit checking
material (e.g., Fit-Checker) may reveal which areas to relieve.
- Check upper and lower separately for VDO and occlusion,
and then together.
- Major faults: repeat final impressions.
- Minor faults: adjust at finish.
- Make new occlusal record, if required.
- Select tooth mold and shade.
- Use altered cast technique, if required.
8. Wax try-in
- Check position of denture teeth.
- Check flange extensions/thickness.
- Check VDO, arch form, occlusal plane and occlusion.
- Check aesthetics with patient and only proceed when
patient is satisfied.
- Prescribe post-dam relief areas and management of
undercuts.
9. Finish once any fitting surface roughness is eliminated, the
dentures are tried in separately, adjusting undercuts and contacts as required.
The extension, occlusion, and articulation are then adjusted if necessary. Give
the patient written and verbal instructions, and a further appointment.









click here
ReplyDeleteanyone with dentures would benefit from reading this article.
Looking for Dentist in Mesa,AZ? Click to learn why we are best dental implant provider. Dental implants are a beautiful, permanent solution to missing teeth! Call us today! We serve patients all over in Mesa.
ReplyDeleteHey! I was looking for information on how much do dental implants cost and found out you can get original dental implants (no knock off) for $1,200 USD with the crown and the abutment included. No kidding. I'm planning my vacation in Cancun and get them set as soon as I can. I'll go back later in a few months for the rehabilitation. Wish me luck! Atte: dental implant vacations
ReplyDeleteQuickly this site will indisputably be famous among all blogging people, because of its fastidious articles or reviews.dentures
ReplyDeleteuseful information on topics that plenty are interested on for this wonderful post.Admiring the time and effort you put into your b!.. alginates
ReplyDeleteAre removable partial dentures comfortable?
ReplyDeleteThe newer flexible removable partial dentures (RPDs) are being used more and more commonly for temporary ,or on occasion permanent, replacement of missing teeth. These dentures are providing a comfortable and successful alternative to traditional RPDs.Jain Dental Clinic promises to deliver quality dental care treatment in Indirapuram, Dentist in East Delhi