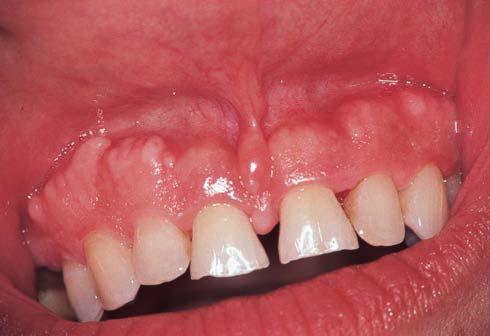
Enamel
Infraction
Definition: incomplete fracture
(crack) of the enamel without loss of tooth structure.
Diagnosis: normal gross
anatomic and radiographic appearance; craze lines apparent, especially with
transillumination.
Treatment objectives: to
maintain structural integrity and pulp vitality.
General prognosis:
Complications are unusual.
Crown
fracture–uncomplicated
Definition: an enamel fracture
or an enamel-dentin fracture that does not involve the pulp.
Diagnosis: clinical and/or
radiographic findings reveal a loss of tooth structure confined to the enamel
or to both the enamel and dentin.
Treatment objectives: to
maintain pulp vitality and restore normal esthetics and function. Injured lips,
tongue, and gingiva should be examined for tooth fragments. When looking for
fragments in soft tissue lacerations, radiographs are recommended. For small
fractures, rough margins and edges can be smoothed. For larger fractures, the
lost tooth-structure can be restored.
General prognosis: The prognosis of uncomplicated
crown fractures depends primarily upon the concomitant injury to the
periodontal ligament and secondarily upon the extent of dentin exposed. Optimal
treatment results follow timely assessment and care.
Crown
fracture–complicated
Definition: an enamel-dentin
fracture with pulp exposure.
Diagnosis: clinical and
radiographic findings reveal a loss of tooth structure with pulp exposure.
Treatment objectives: to
maintain pulp vitality and restore normal esthetics and function. Injured lips,
tongue, and gingiva should be examined for tooth fragments. When looking for
fragments in soft tissue lacerations, radiographs are recommended.
• Primary teeth: Decisions often are based on life expectancy
of the traumatized primary tooth and vitality of the pulpal tissue. Pulpal
treatment alternatives are pulpotomy, pulpectomy, and extraction.
• Permanent teeth: Pulpal treatment alternatives are direct
pulp capping, partial pulpotomy, full pulpotomy, and pulpectomy (start of root
canal therapy). There is increasing evidence to suggest that utilizing
conservative vital pulp therapies for mature teeth with closed apices is as
appropriate a management technique as when used for immature teeth with open
apices.
General prognosis:
The prognosis of crown fractures appears to depend primarily upon a concomitant
injury to the periodontal ligament. The age of the pulp exposure, extent of dentin
exposed, and stage of root development at the time of injury secondarily affect
the tooth’s prognosis. Optimal treatment results follow timely assessment and
care.
Crown/root fracture

Definition: an enamel, dentin,
and cementum fracture with or without pulp exposure.
Diagnosis: Clinical findings
usually reveal a mobile coronal fragment attached to the gingiva with or
without a pulp exposure. Radiographic findings may reveal a radiolucent oblique
line that comprises crown and root in a vertical direction in primary teeth and
in a direction usually perpendicular to the central radiographic beam in
permanent teeth. While radiographic demonstration often is difficult, root fractures
can only be diagnosed radiographically.
Treatment objectives: to
maintain pulp vitality and restore normal esthetics and function.
• Primary teeth: When the primary tooth cannot or should not
be restored, the entire tooth should be removed unless retrieval of apical fragments
may result in damage to the succedaneous tooth.
• Permanent teeth: The emergency treatment objective is to
stabilize the coronal fragment. Definitive treatment alternatives are: to
remove the coronal fragment followed by a supragingival restoration or
necessary gingivectomy, osteotomy, or extrusion (surgical or orthodontic) to
prepare for restoration. If the pulp is exposed, pulpal treatment alternatives
are pulp capping, pulpotomy, and root canal treatment.
General prognosis:
Although the treatment of crown-root fractures can be complex and laborious,
most fractured permanent teeth can be saved. Fractures extending significantly
below the gingival margin may not be restorable.
Root
fracture
Definition: a dentin and cementum
fracture involving the pulp.
Diagnosis: Clinical findings
reveal a mobile coronal fragment attached to the gingiva that may be displaced.
Radiographic findings may reveal 1 or more radiolucent lines that separate the
tooth fragments in horizontal fractures. Multiple radiographic exposures at
different angulations may be required for diagnosis. A root fracture in a
primary tooth may be obscured by a succedaneous tooth.
Treatment objectives:
• Primary teeth: Treatment alternatives include extraction of coronal fragment
without insisting on removing apical fragment or observation. It is not
recommended to reposition and stabilize the coronal fragment.
• Permanent teeth: Reposition and stabilize the coronal fragment in its anatomically
correct position as soon as possible to
optimize healing of the periodontal ligament and neurovascular supply while
maintaining esthetic and functional integrity.
General prognosis:
Pulp necrosis in root-fractured teeth is attributed to displacement of the
coronal fragment and mature root development. In permanent teeth, the location
of the root fracture has not been shown to affect pulp survival after injury.
Therefore, preservation of teeth with root fractures occurring in the tooth’s
cervical third should be attempted. Young age, immature root formation, positive
pulp sensitivity at time of injury, and approximating the dislocation within 1 mm have been found
to be advantageous to both pulpal healing and hard tissue repair of the
fracture.
Concussion
Definition: injury to the
tooth-supporting structures without abnormal loosening or displacement of the
tooth.
Diagnosis: Because the periodontal
ligament absorbs the injury and is inflamed, clinical findings reveal a tooth
tender to pressure and percussion without mobility, displacement, or sulcular
bleeding. Radiographic abnormalities are not expected.
Treatment objectives: to
optimize healing of the periodontal ligament and maintain pulp vitality.
General prognosis:
For primary teeth, unless associated infection exists, no pulpal therapy is
indicated. Although there is a minimal risk for pulp necrosis, mature permanent
teeth with closed apices may undergo pulpal necrosis due to associated injuries
to the blood vessels at the apex and, therefore, must be followed carefully.
Subluxation
Definition: injury to
tooth-supporting structures with abnormal loosening but without tooth
displacement.
Diagnosis: Because the
periodontal ligament attempts to absorb the injury, clinical findings reveal a
mobile tooth without displacement that may or may not have sulcular bleeding.
Radiographic abnormalities are not expected.
Treatment objectives: to
optimize healing of the periodontal ligament and neurovascular supply.
• Primary teeth: The tooth should be followed for pathology.
• Permanent teeth: Stabilize the tooth and relieve any occlusal
interferences. For comfort, a flexible splint can be used. Splint for no more
than 2 weeks.
General prognosis:
Prognosis is usually favorable. The primary tooth should return to normal
within 2 weeks. Mature permanent teeth with closed apices may undergo pulpal necrosis
due to associated injuries to the blood vessels at the apex and, therefore,
must be followed carefully.
Lateral
luxation
Definition: displacement of the
tooth in a direction other than axially. The periodontal ligament is torn and
contusion or fracture of the supporting alveolar bone occurs.
Diagnosis: Clinical findings
reveal that a tooth is displaced laterally with the crown usually in a palatal
or lingual direction and may be locked firmly into this new position. The tooth
usually is not mobile or tender to touch. Radiographic findings reveal an
increase in periodontal ligament space and displacement of apex toward or
though the labial bone plate.
Treatment objectives:
• Primary teeth: to allow passive or spontaneous repositiong
if there is no occlusal interference. When there is occlusal interference, the
tooth can be gently repositioned or slightly reduced if the interference is
minor. When the injury is severe or the tooth is nearing exfoliation, extraction
is the treatment of choice.
• Permanent teeth: to reposition as soon as possible and then
to stabilize the tooth in its anatomically correct position to optimize healing
of the periodontal ligament and neurovascular supply while maintaining esthetic
and functional integrity. Repositioning of the tooth is done with digital
pressure and little force. A displaced tooth may need to be extruded to free
itself from the apical lock in the cortical bone plate. Splinting an additional
2 to 4 weeks may be needed with breakdown of marginal bone.
General prognosis:
Primary teeth requiring repositioning have an increased risk of developing pulp
necrosis compared to teeth that are left to spontaneously reposition. In mature
permanent teeth with closed apices, pulp necrosis and pulp canal obliteration
are common healing complications while progressive root resorption is less
likely to occur.
Intrusion
Definition: apical displacement
of tooth into the alveolar bone. The tooth is driven into the socket,
compressing the periodontal ligament and commonly causes a crushing fracture of
the alveolar socket.
Diagnosis: Clinical findings
reveal that the tooth appears to be shortened or, in severe cases, it may
appear missing. The tooth’s apex usually is displaced labially toward or
through the labial bone plate in primary teeth and driven into the alveolar
process in permanent teeth. The tooth is not mobile or tender to touch. Radiographic
findings reveal that the tooth appears displaced apically and the periodontal ligament
space is not continuous. Determination of the relationship of an intruded primary
tooth with the follicle of the succedaneous tooth is mandatory. If the apex is
displaced labially, the apical tip can be seen radiographically with the tooth
appearing shorter than its contralateral. If the apex is displaced palatally
towards the permanent tooth germ, the apical tip cannot be seen radiographically
and the tooth appears elongated. An extraoral lateral radiograph also can be
used to detect displacement of the apex toward or though the labial bone plate.
An intruded young permanent tooth may mimic an erupting tooth.
Treatment objectives:
• Primary teeth: to allow spontaneous reeruption except when
displaced into the developing successor. Extraction is indicated when the apex
is displaced toward the permanent tooth germ.
• Permanent teeth: to reposition passively (allowing re-eruption
to its preinjury position), actively (repositioning with traction), or
surgically and then to stabilize the tooth with a splint for up to 4 weeks in
its anatomically correct position to optimize healing of the periodontal
ligament and neurovascular supply while maintaining esthetic and functional
integrity. For immature teeth with more eruptive potential (root ½ to ²/³
formed), the objective is to allow for spontaneous eruption. In mature teeth,
the goal is to reposition the tooth with orthodontic or surgical extrusion and initiate endodontic treatment
within the first 3 weeks of the traumatic incidence.
General prognosis: In
primary teeth, 90% of intruded teeth will re-erupt spontaneously (either
partially or completely) in 2 to 6 months. Even in cases of complete intrusion
and displacement of primary teeth through the labial bone plate, a
retrospective study showed the reeruption and survival of most teeth for more
than 36 months. Ankylosis may occur, however, if the periodontal ligament of
the affected tooth was severely damaged, thereby delaying or altering the eruption
of the permanent successor. In mature permanent teeth with closed apices, there
is considerable risk for pulp necrosis, pulp canal obliteration, and
progressive root resorption. Immature permanent teeth that are allowed to
reposition spontaneously demonstrate the lowest risk for healing complications.
Extent of intrusion (7 mm or greater) and adjacent intruded teeth have a
negative influence on healing.
Extrusion
Definition: partial displacement
of the tooth axially from the socket; partial avulsion. The periodontal
ligament usually is torn.
Diagnosis: Clinical findings
reveal that the tooth appears elongated and is mobile. Radiographic findings
reveal an increased periodontal ligament space apically.
Treatment objectives:
•Primary teeth: to
allow tooth to reposition spontaneously or reposition and allow for healing for
minor extrusion (<3 mm) in an immature developing tooth. Indications for an
extraction include severe extrusion or mobility, the tooth is nearing exfoliation,
the child’s inability to cope with the emergency situation, or the tooth is
fully formed.
• Permanent teeth: to reposition as soon as possible and then
to stabilize the tooth in its anatomically correct position to optimize healing
of the periodontal ligament and neurovascular supply while maintaining esthetic
and functional integrity. Repositioning may be accomplished with slow and
steady apical pressure to gradually displace coagulum formed between root apex
and floor of the socket. Splint for up
to 2 weeks.
General prognosis:
There is a lack of clinical studies evaluating repositioning of extruded
primary teeth.6 In permanent mature teeth with closed apices, there is
considerable risk for pulp necrosis and pulp canal obliteration. These teeth must
be followed carefully.
Avulsion
Definition: complete displacement
of tooth out of socket. The periodontal ligament is severed and fracture of the
alveolus may occur.
Diagnosis: Clinical and radiographic
findings reveal that the tooth is not present in the socket or the tooth
already has been replanted. Radiographic assessment will verify that the tooth is not intruded when the tooth was
not found.
Treatment objectives:
•Primary teeth: to prevent further injury to the developing
successor. Avulsed primary teeth should not be replanted because of the potential
for subsequent damage to developing permanent tooth germs.
• Permanent teeth: to replant as soon as possible and then
to stabilize the replanted tooth in its anatomically correct location to optimize healing of the
periodontal ligament and neurovascular
supply while maintaining esthetic and functional integrity except when
replanting is contra-indicated by:
1. The child’s
stage of dental development (risk for ankylosis where considerable alveolar
growth has to take place);
2. Compromising
medical condition; or
3. Compromised
integrity of the avulsed tooth or supporting tissues.
Flexible splinting
for 2 weeks is indicated. Tetanus prophylaxis
and antibiotic coverage should be considered. Treatment strategies are directed
at avoiding inflammation that may occur as a result of the tooth’s attachment
damage and/or pulpal infection.
General prognosis:
Prognosis in the permanent dentition is primarily dependent upon formation of
root development and extraoral dry time. The tooth has the best prognosis if
replanted immediately. If the tooth cannot be replanted within 5 minutes, it
should be stored in a medium that will help maintain vitality of the periodontal
ligament fibers. The best (ie, physiologic) transportation media for avulsed
teeth include (in order of preference) Viaspan, Hank’s Balanced Salt Solution
(tissue culture medium), and cold milk. Next best would be a non-physiologic medium
such as saliva (buccal vestibule), physiologic saline, or water. Although water is detrimental to
cell viability due to its low osmolality and long term storage (ie, more than
20 minutes) in water has an adverse effect on periodontal ligament healing, it
is a better choice than dry storage. Limited tooth storage in a cell-compatible
medium prior to replantation has produced similar healing results as compared
with immediately-replanted teeth.
The risk of ankylosis increases significantly with an
extraoral dry time of 20 minutes An extraoral dry time of 60 minutes is
considered the point where survival of the root periodontal cells is unlikely.
In permanent avulsed teeth, there is considerable risk for pulp necrosis, root
resorption, and ankylosis.
Additional considerations:
Recent evidence suggests that success of replantation is dependent upon many
factors, some of which the clinician can manipulate in a manner that favors
more successful outcomes. Decision trees for acute management of avulsed
permanent incisors have been developed with up-to-date information in an easy
to use flowchart format.
Revascularization: An
immature (ie, open apex) tooth has the
potential to establish revascularization when there is a minimum of a 1.0 mm
apical opening. Complete pulpal revascularization has been shown to occur at a
rate of 18% among immature teeth. It appears that antibiotic treatment reduces
contamination of the root surface and/or pulp space, thereby creating a biological
environment that aids revascularization. On the other hand, a mature tooth (ie,
closed apex or apical opening <1 mm) has little or no chance of
revascularization. Researchers have demonstrated that immature teeth soaked in
doxycycline solution have a greater rate of pulp revascularization.
Periodontal ligament (PDL) management –
transitional therapy: When a tooth has been out of the oral cavity and in a dry
environment for greater than 60 minutes, the PDL has no chance of survival. If
such a tooth is replanted, it is likely to undergo osseous replacement
resorption and, over time, the tooth will become ankylosed and ultimately will
be lost. Because pediatric dentists need to consider the growth and development
of the child patient, the goal for a tooth that has been avulsed for greater
than 60 minutes with dry storage is to delay the osseous replacement and, hence,
ankylotic process as long as possible. To slow down this process, the remaining
PDL should be removed because otherwise it becomes a stimulus for inflammation that
accelerates infection-related resorption. The remaining PDL can be removed by
several methods: gentle scaling and root planning, soft pumice prophylaxis,
gauze, or soaking the tooth in 3% citric acid for 3 minutes. This should be
followed by a sodium fluoride treatment for 20 minutes. The rationale for this
fluoride soak is based upon evidence that this procedure will delay, but not
prevent, ankylosis; fluoroapatite is more resistant to ankylosis than
hydroxy-apatite. When teeth are soaked in fluoride before replantation, it has
been shown to reduce significantly the risk of resorption after a follow-up of
5 years. Despite these recommendations, teeth that have been out of the oral cavity for greater than 60 minutes with
dry storage have a poor prognosis and
will not survive long term.
Possible contraindications to replantation:
There are possible contraindications to tooth replantation. Examples are immunocompromised health, severe congenital
cardiac anomalies, severe uncontrolled seizure disorder, severe mental disability,
severe uncontrolled diabetes, and lack of alveolar integrity.
Current research:
Antiresorptive-regenerative therapies may have potential for enhancing the
prognosis of avulsed teeth.
Treatment strategies are directed at avoiding or
minimizing inflammation, increasing revascularization, and producing hard
barriers in teeth with open apices. New treatment strategies also are directed
at specific clinical challenges that include decoronation as an approach to
treat ankylosis in growing children and transplantation of premolars as an approach
for replacing avulsed teeth. Dental practitioners should follow current
literature and consider carefully evidence-based recommendations that may enhance
periodontal healing and revascularization of avulsed permanent teeth.